Sleep Science Friday (24/7/2020)
Sleep Science Friday
Yes! It’s Friday! Grab a coffee (or tea) and end your week with some Sleep Science News and ESRS updates!
What’s keeping you up? The European Insomnia Network and CBT-I
(24 July 2020)
Almost everyone has experienced sleepless nights—waking up the next day cranky, exhausted and unable to focus. For some, this is a rare occurrence; while for others, it appears with regularity. This is insomnia: a fairly common, but neglected, condition that makes it difficult to fall and stay asleep. Sometimes lasting only a few days or weeks (acute)—usually as a response to stress or trauma—insomnia can also persist for months or longer (chronic).
Lack of sleep doesn’t just make you tired, it comes with a myriad of health consequences, with primary insomnia as a precursor to other conditions (including depression and increased suicide risk, as well as cardiovascular diseases and higher risk of cancer). Insomnia can also occur secondary alongside psychiatric disorders (e.g. depression, anxiety, substance abuse, bipolar disorder) and general medical conditions (e.g. cancer, chronic pain, neurological disease, chronic obstructive pulmonary disease) that can create a feedback loop of deteriorating health.
With varying estimates of prevalence among different populations (from as low as 5%, to as high as 33%, or even 50%), insomnia unequivocally affects millions each year—burdening healthcare systems in terms of costs and manpower. Despite being widespread, insomnia research and its non-pharmaceutical treatments are still under funded in comparison to other medical or psychiatric conditions as insomnia commonly presents alongside more critical conditions (e.g. Alzheimer’s disease). Insurance companies may also not cover insomnia treatments unless the patient has comorbid conditions, such as depression. Although, given the link between insomnia and immune system activation, memory and learning, and emotional regulation, directly treating insomnia may help prevent or alleviate certain psychological and physical conditions.
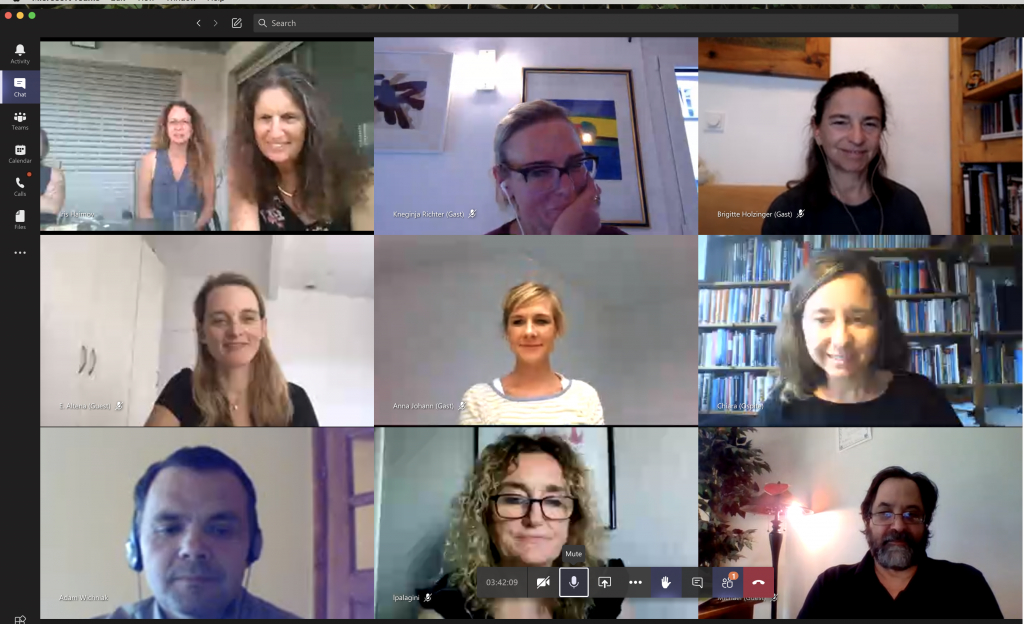
To address this gap, the European Insomnia Network (EIN), established in 2009, held a virtual meeting 16 July 2020 to discuss insomnia treatments and research in Europe. With 29 members attending, Dr. Dieter Riemann (chair of the EIN) opened the floor for discussion, including future plans of the EIN (Prof. Dr. Kai Spegelhalder) and the Cognitive Behavioural Therapy for Insomnia (CBT-I) Academy in Europe (Dr. Colin Espie and Dr. Chiara Baglioni) and collaborations in the USA (Dr. Michael Perlis); followed by talks on insomnia and COVID-19 (Baglioni), women and pregnancy (Dr. Laura Palagini), postural gait in the elderly (Prof. Iris Haimov), and repetitive thinking and depression/anxiety (Dr. Andrea Ballesio); as well as sleep certification and CBT-I in Portugal (Joanna Isaac, MD).
Currently, the first line of insomnia treatment is practicing good “sleep hygiene” (e.g. no screens before bed, no caffeine in the evenings, the bed is only for sleeping), with the possible addition of prescribed sedative-hypnotic drugs (e.g. Ambien). Although creating good habits can be helpful, it does not go far enough in addressing the root causes of insomnia—for example, you would not tell someone with depression to just exercise more. Meanwhile, medications may have harmful side effects and can create dependencies. Therefore, the EIN believes that CBT-I should be the first-line in insomnia treatment.
CBT-I targets factors that lead to chronic insomnia, such as “dysregulation of the sleep drive, sleep-interfering behaviours and cognitions, attempts to control the sleep process and sleep-related anxiety”. Treatments typically include “stimulus control therapy, sleep restriction therapy and a range of cognitive therapeutics, supplemented by psychoeducation/sleep hygiene and relaxation training”. Therapy is adjusted to individual patient needs and requires bridging methods and knowledge between behavioral therapists and clinicians.
However, currently, there is a lack of standardization in CBT-I—with results varying significantly from patient to patient. Therefore, the European Sleep Research Society (ESRS) and the EIN developed a Task Force in May 2018 to standardize CBT-I treatment plans by establishing the European CBT-I Academy. The Academy also aims to make CBT-I training available with centre accreditation, not only for those working specifically with sleep disorders, but also for social workers, medical staff, psychotherapists, psychologists, and psychiatrists. In this way, they hope to make CBT-I more readily available to those who suffer from insomnia.
With the current COVID-19 crisis, developing effective insomnia treatments has only become more urgent. Acute stressors are known to fundamentally alter sleep, with long-term consequences particularly on mental health. Already seen in children and adults, many have disrupted sleep schedules due to lockdown measures and uncertain situations. Given the link between sleep and health and the wide prevalence of insomnia, funding and researching alternative non-pharmaceutical solutions and promoting CBT-I may help alleviate pressures faced by medical healthcare workers and lessen comorbid conditions for insomnia sufferers.
To hear more about insomnia and health consequences and treatments, the EIN will take part in the ESRS Congress Virtual Edition (22-24 Sept, 2020). Check out the schedule and register before 14 Aug for the Early Bird Registration Fee. We hope to “see” you there
Want to know more about Insomnia and Health? Further Reading:
- “Dealing with sleep problems during home confinement due to the COVID-19 outbreak: Practical recommendations from a task force of the European CBT-I Academy” (4 April 2020, Journal of Sleep Reseach)
- “Caring for the carers: Advice for dealing with sleep problems of hospital staff during the COVID-19 outbreak” (8 June 2020, Journal of Sleep Research)
- “How Covid-19 lockdown has altered sleep in the US and Europe” (10 June 2020, Science Daily)
- “Children’s sleep severely affected by impact of coronavirus, say experts” (17 July 2020, The Guardian)
- “Sleep disturbance and psychiatric disorders” (July 2020, The Lancet)
- “Insomnia during COVID-19 pandemic and lockdown: Prevalence, severity, and associated risk factors in French population” (August 2020, Psychiatry Research)
Join ESRS! We are currently hiring a Business Administrator (50%). Deadline 31 July, 2020.
Just published an article? Want your research to be featured? Saw something interesting? Contact: doris.wu [ at ] esrs.eu to be featured.